
Seeing Is Believing: The Benefits of Ultrasound for Patients and Providers

Fatty Liver Symptoms: Silent Doesn’t Mean Harmless—What People Actually Feel
Fatty Liver Symptoms: Silent Doesn’t Mean Harmless;What People Actually Feel
People call fatty liver “silent,” and that phrase has done more damage than it should. Silent doesn’t mean safe. It means the problem can grow for a long time without obvious warning signs, while your liver quietly carries the load and keeps functioning… until it starts struggling.
That’s what makes fatty liver sneaky.
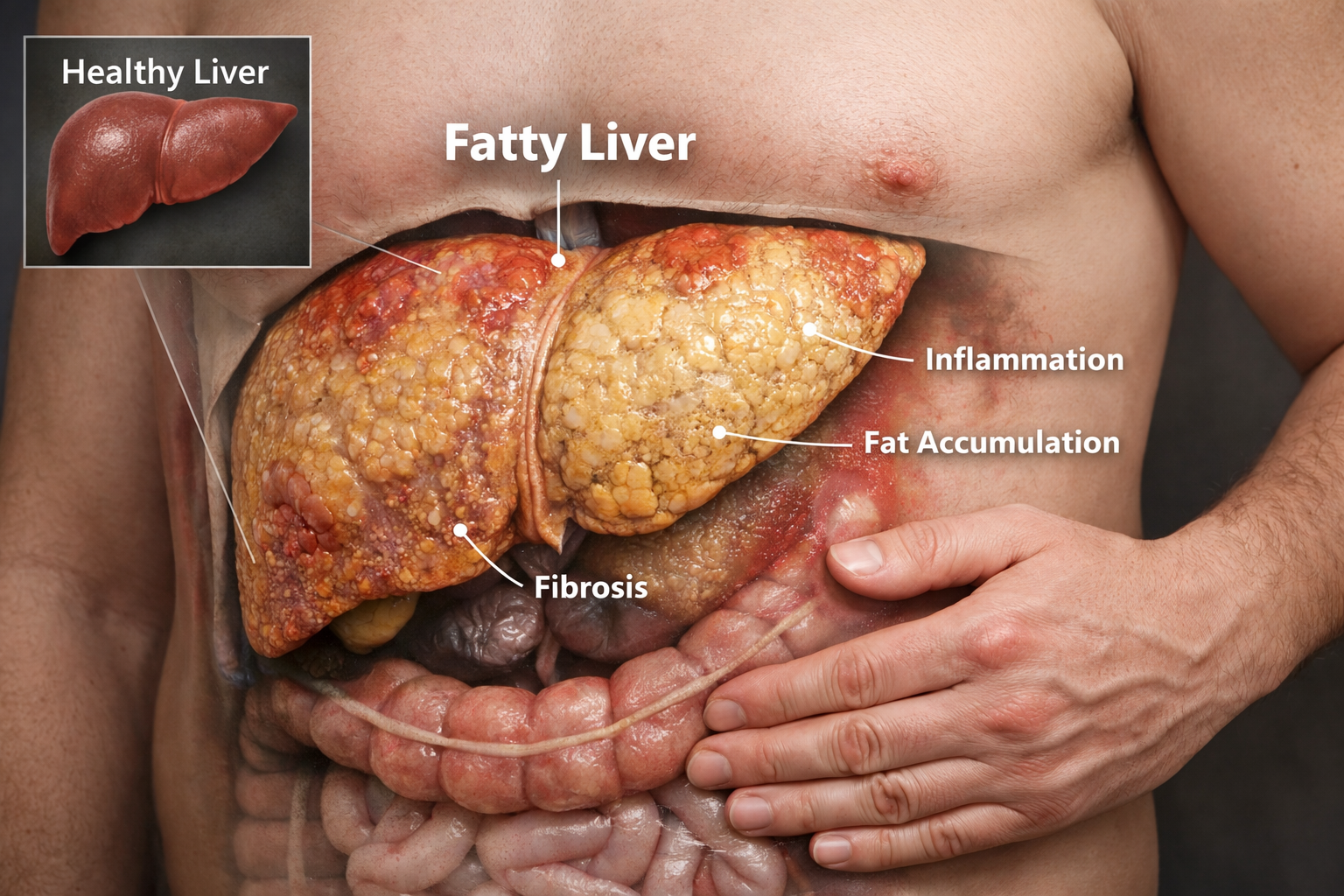
What fatty liver is (and why the name keeps changing)
You will still see the older terms NAFLD and NASH online, but many medical groups now use newer names.
MASLD refers to fatty liver linked to metabolic dysfunction, meaning it’s commonly tied to things like insulin resistance, type 2 diabetes, high cholesterol, high blood pressure, and excess body weight. MASH is the more serious form, where inflammation starts showing up alongside fat in the liver and the risk of scarring rises.
So when people talk about fatty liver, they’re often talking about a bigger issue than fat alone. They’re talking about metabolism, inflammation, and long-term strain.
Why people say it’s silent (and why that’s misleading)
Fatty liver is often discovered accidentally. Someone gets routine bloodwork, or an ultrasound for something unrelated, and the report mentions fatty liver. That’s common because early stages don’t always produce specific symptoms.
But here’s where people get fooled: even when symptoms exist, they’re usually vague. They don’t scream liver problem. They whisper life is stressful,or “maybe I’m just tired.”
And that’s exactly how people ignore it for years.
What people actually feel in the early stages
Many people truly feel nothing. But when symptoms show up, this is what it often looks like in real life.
The first one is fatigue that doesn’t match your effort. It’s that constant drained feeling, like you’re sleeping but not recovering. You wake up tired, you crash easily, and you find yourself running on low power more days than not.
Another common experience is a general feeling of being unwell. Not sick enough to stay in bed, but not well enough to feel sharp. You might describe it as sluggish, heavy, foggy, or just “off.”
Some people also notice a dull ache or discomfort under the right side of the ribs. It’s not always painful. Sometimes it’s just pressure, fullness, or mild discomfort that comes and goes.
Here’s the important part. None of these symptoms are exclusive to fatty liver. Stress, poor sleep, thyroid issues, anemia, gallbladder problems, reflux, depression, and dozens of other conditions can look similar. Symptoms don’t diagnose. Patterns plus risk factors plus testing do.
When fatty liver stops being quiet
Fatty liver becomes dangerous when it progresses into significant inflammation and scarring. That’s where fibrosis and cirrhosis come in, and that’s when symptoms can get more serious.
At that stage, fatigue tends to intensify. You may bruise more easily. Appetite might drop. Nausea can show up. Some people lose weight without trying. Itchy skin can appear and feel relentless. Yellowing of the eyes or skin, known as jaundice, is one of the clearer warning signs that the liver is not doing well.
Swelling becomes another clue. It might show up in the ankles and legs, or as fluid buildup in the abdomen. Some people notice spider-like blood vessels on the skin. Others develop confusion, drowsiness, or mental fog that feels abnormal and unsettling.
If you take nothing else from this post, take this: jaundice, significant belly swelling, vomiting blood, black stools, or confusion are not “let me Google this for a week” symptoms. Those are urgent.
Who should pay attention even without symptoms
Fatty liver is much more likely when certain risk factors are present.
If you carry more weight around your midsection, if you have type 2 diabetes or prediabetes, if your cholesterol or triglycerides are high, or if your blood pressure is elevated, your odds go up. PCOS also increases risk. Age matters too, especially after 50.
Even if you feel fine, checking several of those boxes means you shouldn’t assume everything is okay. A silent condition plus risk factors is not peace. It’s uncertainty.
How fatty liver is usually found
Most people find out through blood tests, imaging, or both.
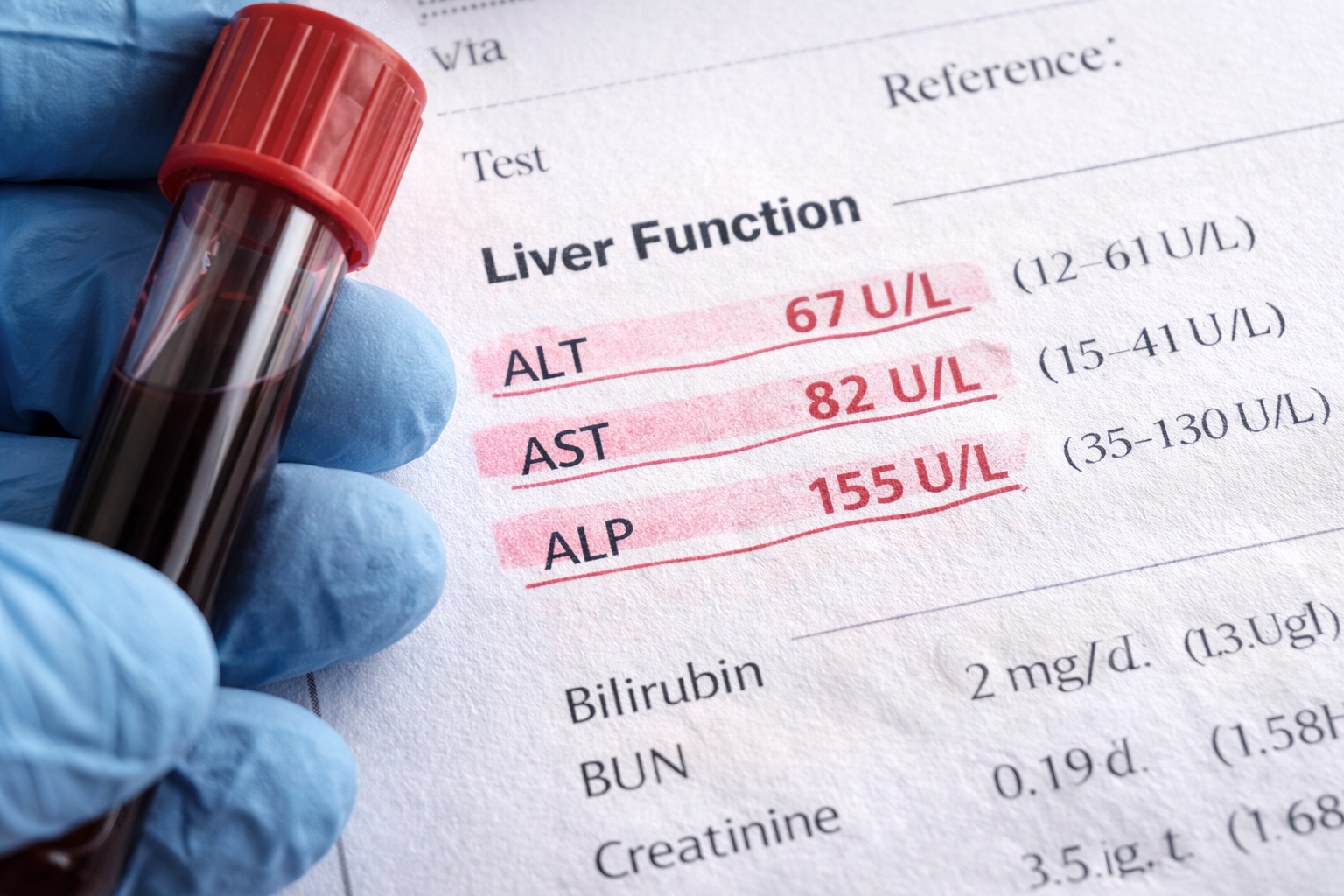
Bloodwork may show elevated liver enzymes, although this is not guaranteed. Some people have fatty liver with normal enzymes, which is why “my labs are fine” is not the victory lap people think it is.
Imaging like an abdominal ultrasound can detect fat in the liver. But ultrasound doesn’t always tell the whole story, because the real danger isn’t just fat. It’s inflammation and scarring. That’s why clinicians sometimes use additional tests to assess fibrosis when someone’s risk is higher.
The uncomfortable truth: what actually helps
There’s no detox tea powerful enough to reverse metabolic dysfunction. The liver doesn’t need a cleanse. It needs fewer repeated hits.
If someone is overweight, weight loss is one of the most effective levers. Even modest loss can reduce fat in the liver. Greater loss is often needed to reduce inflammation and scarring. Exercise helps too, even when weight doesn’t change much, because movement improves insulin sensitivity and metabolic health.
Consistency matters more than intensity. Crash diets are not the move here. Rapid weight loss can actually worsen liver problems in some situations.
This is also where people get trapped in scams. Supplements are not automatically safe just because they’re natural. Some can damage the liver. If you’re already worried about your liver, randomly experimenting with herbs is not “holistic.” It’s reckless.
A simple reality check
You should consider getting evaluated if you have persistent fatigue that doesn’t make sense, especially if you also have metabolic risk factors. Same if you keep noticing discomfort under the right ribs, or if your labs or imaging have ever mentioned fatty liver.
The goal isn’t to panic. The goal is to stop living in guesswork.
For those seeking expert ultrasound services, Atlanta Ultrasound offers quick, efficient, and comprehensive scans. Our team of skilled professionals is dedicated to providing you with the clarity and care you need.
Contact us today to schedule your ultrasound scan and take a decisive step towards understanding your health.
📍 Multiple locations in Metro Atlanta, GA
📞 Contact: 678-590-3300
🌐 Website:www.atlantaultrasound.com
Disclaimer: The content of this blog post, authored by a sonographer, is provided for educational and informational purposes only. It is not intended as medical advice, nor should it substitute for professional medical consultation, diagnosis, or treatment. Always seek the advice of your physician or other qualified health providers with any questions you may have regarding a medical condition or health concerns.
