
Seeing Is Believing: The Benefits of Ultrasound for Patients and Providers
CIMT Scan 101: What It Measures and Why It’s a Big Deal for Prevention
CIMT Scan 101: What It Measures and Why It’s a Big Deal for Prevention
Most heart and stroke problems don’t show up with a dramatic warning sign. They build quietly, over years, while you feel “fine.” That’s why prevention is everything… and why tests that can spot early artery changes get so much attention.
One of the most talked-about options is the CIMT scan. Here’s what it is, what it actually measures, what it can and can’t tell you, and why it matters if you care about prevention.
What is a CIMT scan?
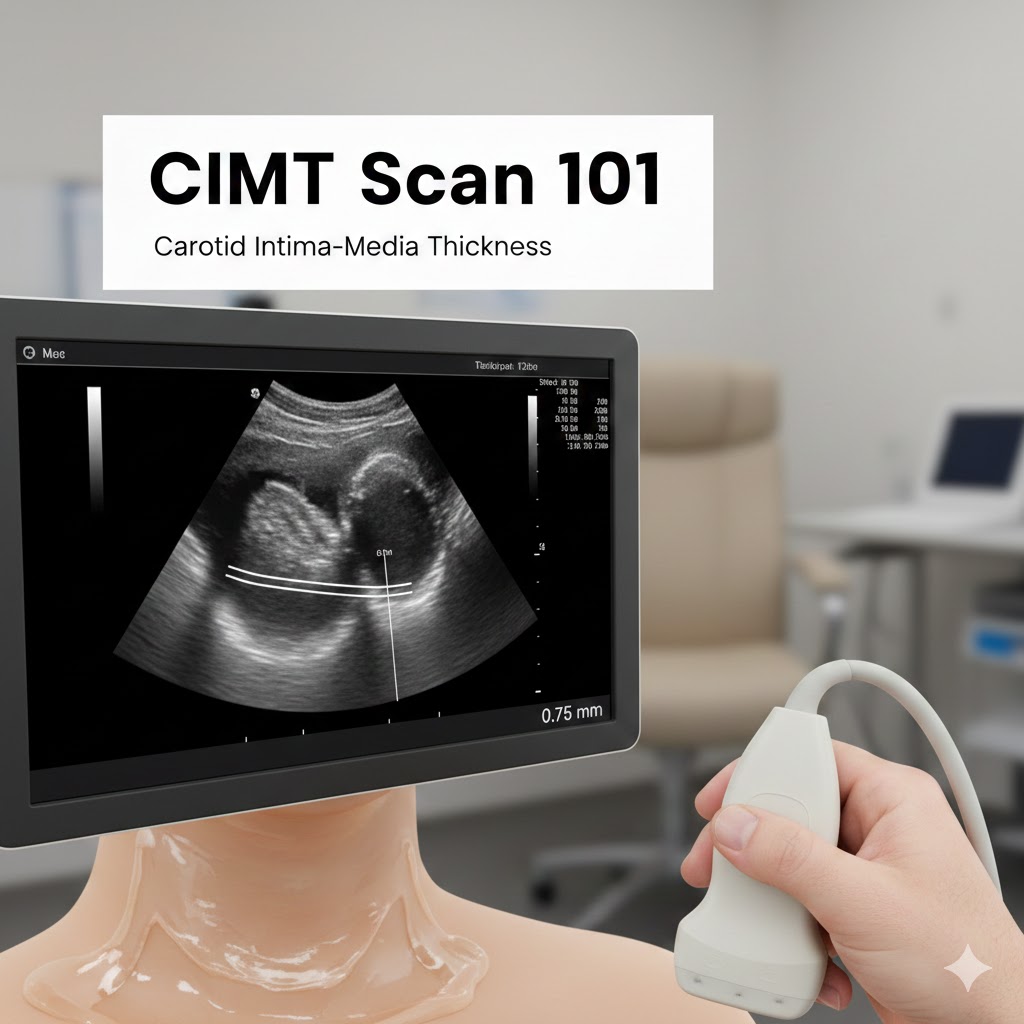
CIMT stands for Carotid Intima-Media Thickness.
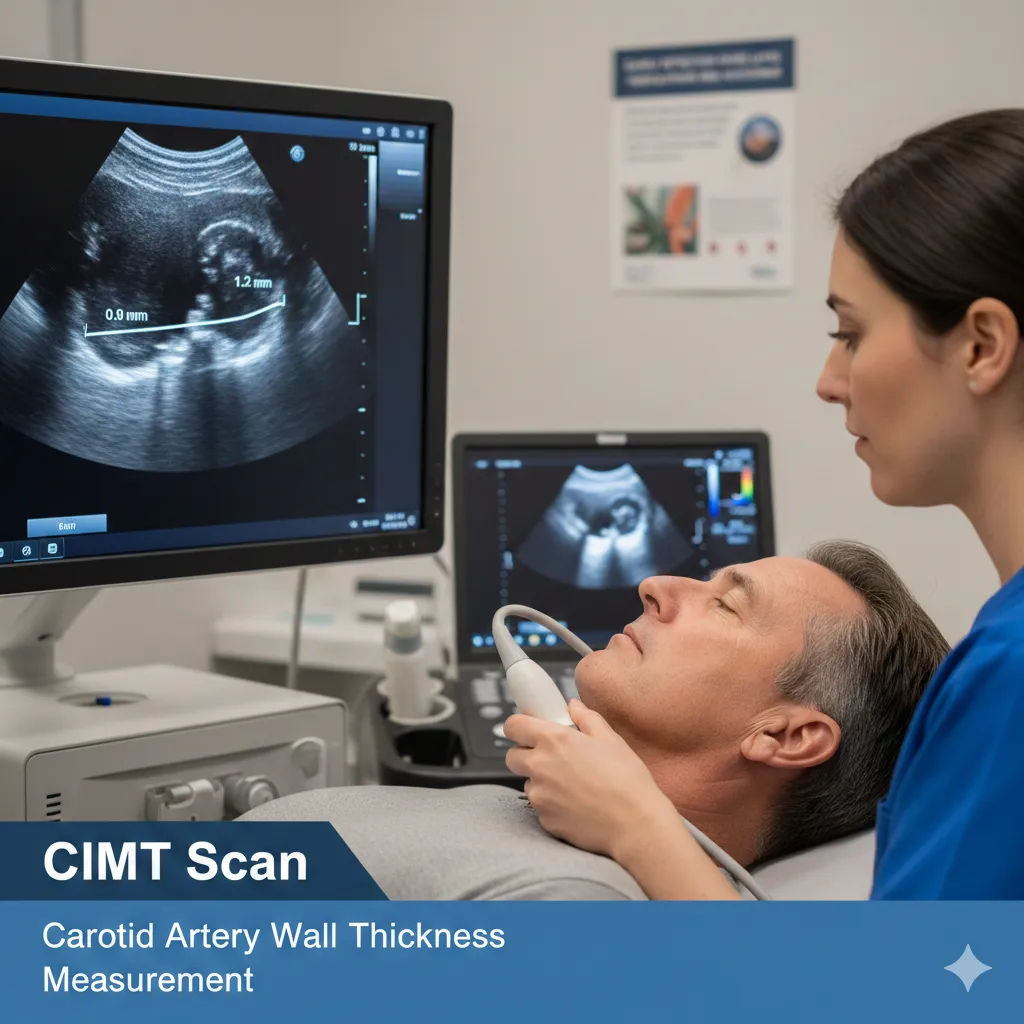
A CIMT scan is a non-invasive ultrasound test done on the neck. It looks at your carotid arteries—the major blood vessels that carry oxygen-rich blood to your brain—and measures how thick the inner artery wall layers are. Those two layers are called the intima (inner layer) and media (middle layer).
Why measure thickness? Because arteries tend to get thicker as plaque builds and atherosclerosis develops. That thickening can show up before you have symptoms.
What does a CIMT scan measure, exactly?
A CIMT scan measures:
1) Artery wall thickness (IMT)
This is the “thickness number” that reflects changes in the artery wall over time. Increased thickness can be associated with higher cardiovascular risk.
2) Sometimes: plaque
Many carotid ultrasound approaches also look for plaque presence (not just thickness). Plaque tends to be especially meaningful for risk prediction—often more than thickness alone.
Important reality check: CIMT is not the same thing as diagnosing a dangerous blockage. It’s generally about early vessel changes and plaque, not “you have a 90% blockage” findings (that’s a different kind of carotid ultrasound evaluation).
Why prevention people care about CIMT
Because it can help answer a brutally practical question:
Are my arteries aging faster than they should?
Traditional risk checks—cholesterol, blood pressure, A1C, family history are essential. But they’re still risk factors, not a direct look at your artery walls.
A CIMT scan is appealing because it can:
Detect early artery wall changes linked to atherosclerosis
Flag higher risk for events like heart attack and stroke (especially when plaque is seen)
Create motivation: people often take prevention more seriously when they can see what’s happening

What the test is like ?
A trained ultrasound professional places a small probe on your neck, and the machine captures images of your carotid arteries. There’s typically little to no prep—wear an open-neck shirt and skip bulky jewelry.
No needles. No radiation. Usually done fast.
Who might benefit most from CIMT?
This is where you need clear thinking, not hype.
CIMT is often considered when someone is:
Not obviously high-risk (already needing aggressive treatment), but also not clearly low-risk
In the “intermediate risk” zone where extra information might change the plan
Has risk factors like high blood pressure, high cholesterol, high blood sugar, smoking history, etc.
A clinician may use CIMT results to decide whether prevention should be more aggressive (lifestyle, medications, follow-up strategy).
The honest truth: CIMT is useful and also debated
Here’s the uncomfortable part most marketing pages skip:
Guidelines have shifted over time.
Earlier guidance supported CIMT in some intermediate-risk situations.
But the 2013 ACC/AHA cardiovascular risk guideline moved against routine CIMT measurement for first-event risk assessment in clinical practice.
Why the hesitation? A few reasons:
Measurement consistency matters (technique and protocol differences can affect results).
Age influences CIMT a lot, which complicates interpretation.
There’s increasing recognition that carotid plaque assessment may outperform CIMT thickness alone for risk stratification.
How to use CIMT results
If your CIMT is reassuring
That’s good—but don’t turn it into an excuse. Prevention still matters because arteries change over time. Use it as confirmation that your current habits and medical plan are working.
If your CIMT shows increased thickness and/or plaque
That’s your early warning signal. The smart response is not panic—it’s precision:
Tighten blood pressure control
Improve cholesterol management (sometimes lifestyle + sometimes meds—your clinician decides)
Address blood sugar/insulin resistance if present
Stop smoking (non-negotiable)
Increase consistent movement (walking counts—consistency beats intensity)
Upgrade nutrition (less ultra-processed, more fiber/protein/whole foods)
Prioritize sleep and stress regulation (because inflammation and BP are not vibes-based)
And yes: if the finding is significant, your clinician may recommend additional evaluation or more targeted prevention steps.
One more critical prevention note
There’s a difference between smart, clinician-guided prevention testing and mass screening that creates more harm than help.
For example, the USPSTF recommends against screening for asymptomatic carotid artery stenosis in the general adult population because harms can outweigh benefits.
That’s not a “CIMT ban,” but it is a reminder: screening decisions should be individualized, not marketed like a universal life hack.
Bottom line
A CIMT scan is a simple ultrasound measure of carotid artery wall thickness, sometimes paired with plaque assessment. It can reveal early artery changes linked to cardiovascular risk—often before symptoms appear.
It’s a big deal for prevention when it’s used the right way:
as a supporting tool, not the whole strategy
interpreted in context (age, risk factors, and overall health)
followed by a real plan, not anxiety
For those seeking expert ultrasound services, Atlanta Ultrasound offers quick, efficient, and comprehensive scans. Our team of skilled professionals is dedicated to providing you with the clarity and care you need.
Contact us today to schedule your ultrasound scan and take a decisive step towards understanding your health.
📍 Multiple locations in Metro Atlanta, GA
📞 Contact: 678-590-3300
🌐 Website:www.atlantaultrasound.com
Disclaimer: The content of this blog post, authored by a sonographer, is provided for educational and informational purposes only. It is not intended as medical advice, nor should it substitute for professional medical consultation, diagnosis, or treatment. Always seek the advice of your physician or other qualified health providers with any questions you may have regarding a medical condition or health concerns.
